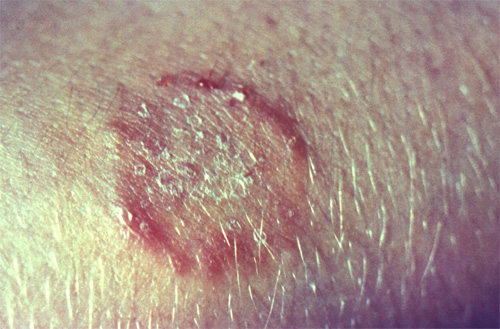
The Centers for Disease Control and Prevention (CDC) has reported two cases of a highly contagious drug-resistant ringworm. These represent the first ever reported cases of the infection in the U.S.
Ringworm (also known as “tinea” and “dermatophytosis”) is a common infection of the skin, hair, or nails. Most cases of ringworm do not lead to severe illness and treatment with antifungal drugs, often terbinafine, usually relieves symptoms and prevents spread to others. However, over the past decade, healthcare providers have reported increasing cases of drug-resistant ringworm. This occurs when germs like bacteria and fungi develop the ability to defeat the drugs designed to kill them. That means the germs are not killed and continue to grow. CDC says the true number of antimicrobial-resistant ringworm cases is difficult to estimate because antifungal susceptibility testing is not widely available and reporting of antimicrobial-resistant ringworm cases is currently not required in the United States.
CDC yesterday revealed details of two cases of drug-resistant ringworm in the United States. On February 28, 2023, a New York City dermatologist notified public health officials of two patients who had severe ringworm that did not improve with oral terbinafine treatment, raising concern. The patients shared no epidemiologic links.
Patient A, a woman aged 28 years, developed a widespread itchy rash during summer 2021. She had a first dermatologic evaluation in December 2021, at which time she was in her third trimester of pregnancy. She had no other underlying medical conditions, no known exposures to a person with similar rash, and no recent international travel history. CDC reports that dermatologists noted “large, annular, scaly, pruritic plaques over the neck, abdomen, pubic region, and buttocks”. She received a diagnosis of ringworm and began oral terbinafine therapy in January 2022 after the birth of her baby. Because her symptoms did not improve after two weeks of therapy, terbinafine was discontinued, and she began itraconazole treatment. The rash resolved completely after completing a 4-week course of itraconazole; however, she is being monitored for potential recurrence of infection and the need for resumption of itraconazole.
Patient B, a woman aged 47 years with no major medical conditions, developed a widespread, itchy rash in summer 2022 while in Bangladesh. There, she received treatment with topical antifungal and steroid combination creams and noted that several family members were experiencing similar eruptions. After returning to the United States, she visited an emergency department three times during autumn 2022. She was prescribed hydrocortisone 2.5% ointment and diphenhydramine (visit 1), clotrimazole cream (visit 2), and terbinafine cream (visit 3) with no improvement. In December 2022, she was evaluated by dermatologists who noted “widespread, discrete, scaly, annular, pruritic plaques affecting the thighs and buttocks”. She received a four-week course of oral terbinafine, but her symptoms did not improve. She then received a four-week course of griseofulvin therapy, resulting in approximately 80% improvement. Itraconazole therapy is being considered pending further evaluation. Her son and husband, who live in the same house and report similar symptoms, are currently undergoing evaluation.
CDC says these two cases highlight several important points. Patient A had no recent international travel history, suggesting potential local U.S. transmission.
Samples from both patients showed the presence of Trichophyton indotineae, which is a dermatophyte mold. This mold often has genetic mutations that make it resistant to antifungal drugs. In India, cases of antimicrobial-resistant ringworm caused by T. indotineae have reached epidemic proportions. Ringworm cases caused by T. indotineae are often severe (covering large regions of the body) and difficult to treat.
CDC says several factors might be contributing to the emergence and spread of antimicrobial-resistant dermatophytes. These include overuse of over-the-counter topical antifungal creams, inappropriate use of topical steroid creams, inappropriate prescription of antifungal drugs, inadequate adherence to prescribed courses of antifungal medication, and global travel and migration.
CDC is calling for healthcare providers to consider T. indotineae infection in patients with widespread ringworm, particularly when symptoms do not improve with first-line topical antifungal agents or oral terbinafine. Culture-based identification techniques used by most clinical laboratories typically misidentify T. indotineae as T. mentographytes or T. interdigitale; correct identification requires genomic sequencing. Healthcare providers who suspect T. indotineae infection should contact their state or local public health department for assistance with testing, which is available at certain public health laboratories and specialized academic and commercial laboratories. CDC also notes that public health surveillance efforts and increased testing could help detect and monitor the spread of T. indotineae in the United States.